Shoulder dislocation: Diagnosis and surgery
Shoulder instability is defined as recurrent dislocations or subluxations (initial dislocation with spontaneous realignment) of the shoulder. These recurrent shoulder dislocations can be treated with re-stabilization surgery using the Latarjet or Bankart technique.
Contents :
What is a shoulder dislocation?
A shoulder dislocation is the displacement of the humeral head out of its joint socket, moving away from the glenoid of the scapula.
It is most often caused by trauma (sports injury or road accident).
Once the shoulder becomes unstable after repeated dislocations, it may dislocate again even during a simple movement or even during sleep.
A shoulder dislocation is usually very painful and leads to near-complete functional incapacity, with inability to move the arm.
Types of shoulder dislocation
The shoulder joint is formed by the humeral head (upper end of the arm bone) articulating with the glenoid, a shallow socket on the scapula. Because this joint is not deeply “socketed,” it relies heavily on ligaments, the joint capsule, and the labrum for stability.
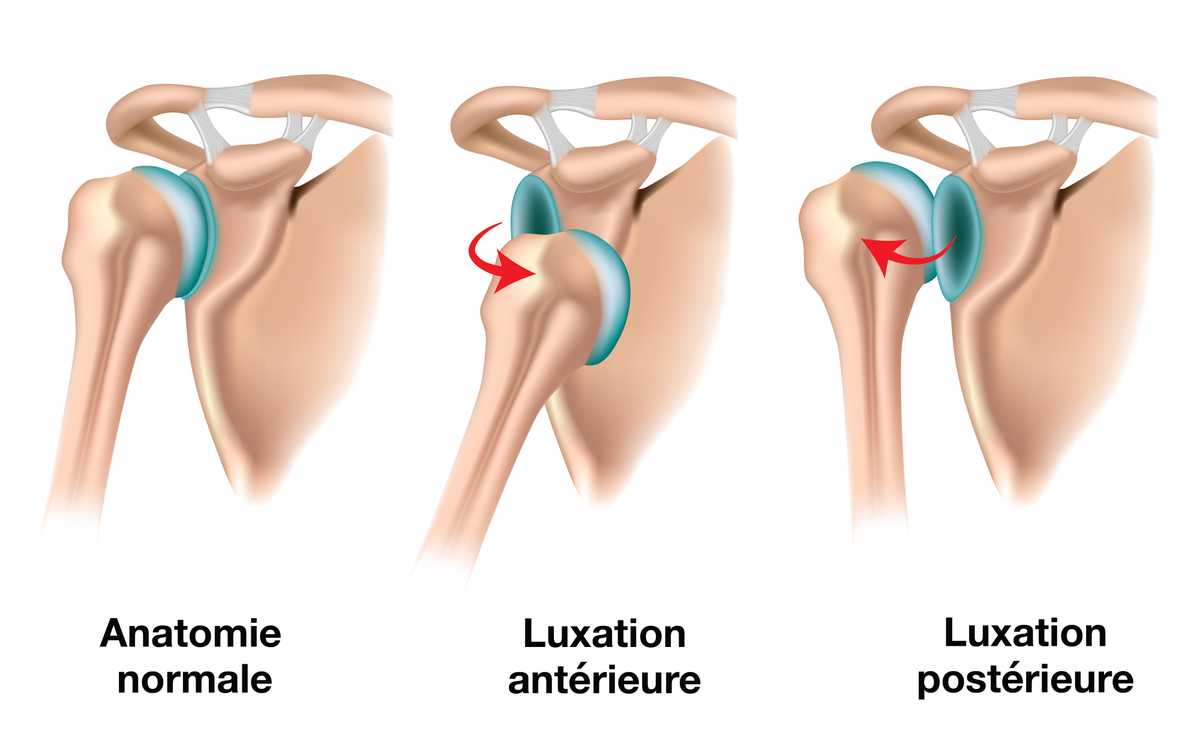
Shoulder dislocations are classified according to the position of the humeral head:
- Anterior dislocation (in front of the glenoid), by far the most common
- Posterior dislocation (behind the glenoid)
- Inferior dislocation (below the glenoid)
Most shoulder dislocations are anterior.
Dislocation and shoulder instability
Shoulder instability is defined after 2 to 3 dislocation episodes. It may also include subluxations, where the joint partially dislocates and spontaneously reduces.
Beyond the pain, instability leads to significant functional limitation. Dislocations may become more frequent and occur with increasingly minor trauma, or even everyday movements.
Patients often develop marked apprehension during at-risk movements (such as overhead arm positioning, like a tennis or handball serve). This leads to self-limitation in daily and sports activities.
Diagnosis of shoulder dislocation
Clinical examination
Diagnosis is primarily made through clinical examination.
Pain is usually intense, and the arm is difficult or impossible to move. A visible deformity or “bump” may appear due to the displaced humeral head.
In cases of chronic instability, the surgeon may reproduce apprehension or pain during abduction and external rotation (overhead arm position). Generalized ligament laxity may also be present.
Imaging
Imaging is often required to confirm diagnosis and assess associated injuries.
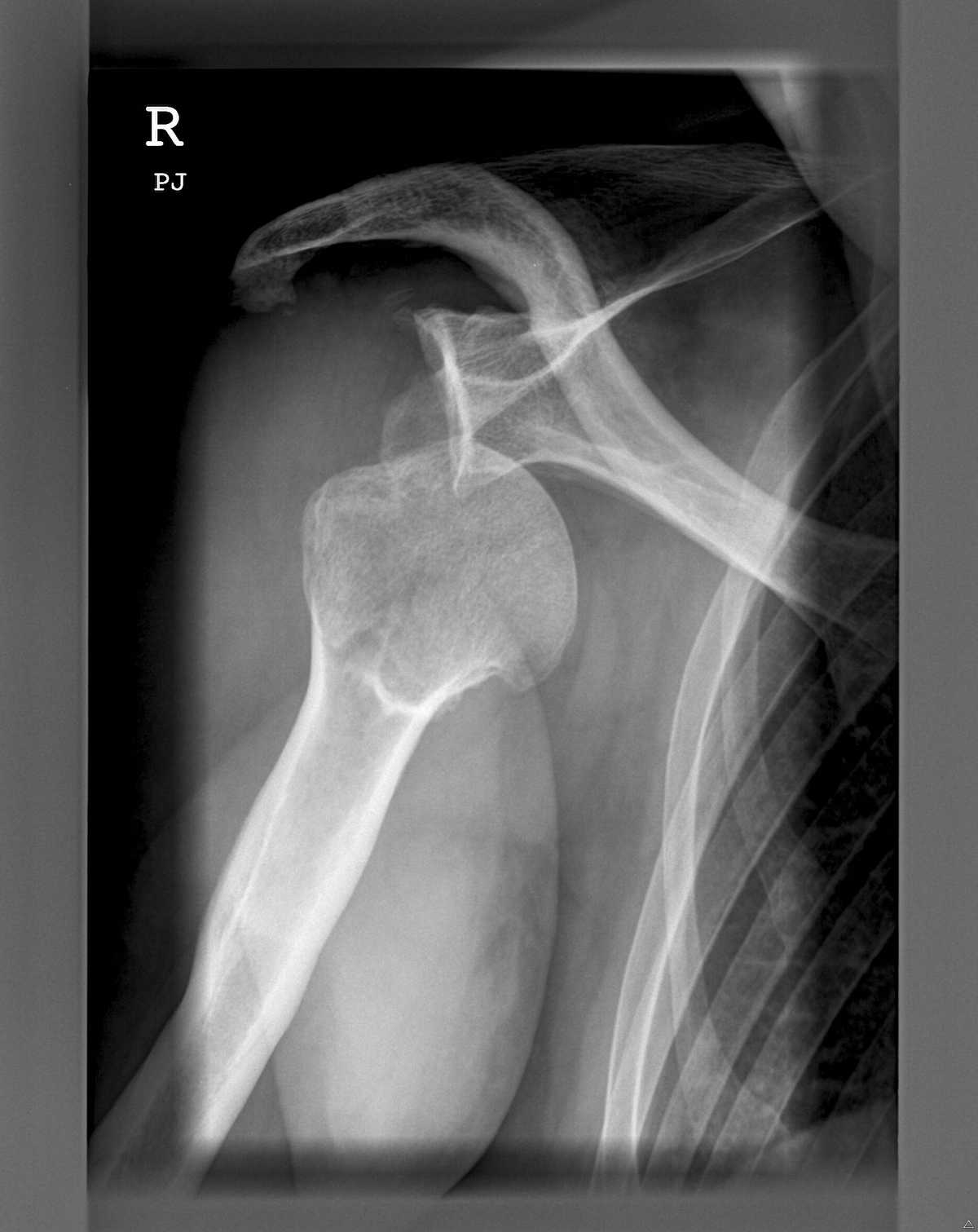
Standard X-rays are used initially, both at the time of dislocation and after reduction.
A CT arthrogram is often performed later to evaluate associated soft tissue damage. It involves injecting contrast into the joint before scanning, allowing visualization of structures not seen on standard imaging.
This exam helps determine whether surgery is required and guides surgical planning.
Should shoulder dislocation be operated on?
After a single dislocation
After a first dislocation, surgery is usually not required. Treatment consists of immobilization and physiotherapy.
Rehabilitation should begin early, respecting healing phases:
- Early phase: pain control and protection of healing structures
- Recovery phase: restoration of range of motion
- Strengthening phase: muscle strengthening and shoulder conditioning
In athletes or in cases of persistent symptoms, imaging (CT arthrogram) may be performed early, and surgery may be considered if there is a high risk of recurrence.
In cases of recurrent instability
After 3 dislocation episodes, surgery is generally recommended. In some cases, it may be considered earlier.
The goal is to prevent recurrence and degenerative joint damage, and to restore normal shoulder function, including return to sports.
Which surgery to stabilize the shoulder?
Surgery is recommended after 2 to 3 dislocations, depending on the patient’s activity level and anatomy.
Two main procedures are used: the Latarjet procedure and the Bankart repair.
Latarjet procedure
The Latarjet procedure involves placing a bone block in front of the glenoid to prevent further dislocation. It also transfers tendons that act as a dynamic stabilizer.
> Learn more about the Latarjet procedure
Bankart repair
The Bankart procedure involves reattaching and tightening the torn labrum and capsule, usually performed arthroscopically.
Arthroscopy is a minimally invasive technique using a camera and small instruments through small incisions. It offers less pain and faster recovery.
> Learn more about Bankart repair
Which surgery should be chosen?
The choice depends on anatomical lesions and patient profile.
During consultation, the advantages and limitations of each technique are explained, and the most appropriate option is selected together with the patient.